Biohazard (bacteria, molds, Legionella)
D. Lgs. 81/08, Annex IV, states that in enclosed workplaces it is necessary to ensure that, taking into account the methods of work and the physical demands on the workers, they have healthy air in sufficient quantity obtained preferentially with natural openings and, when this is not possible, ventilation systems. If a forced ventilation system is used, it must be maintained efficiently working. Any breakdown must be indicated by a control system, when it is necessary to safeguard the health of workers. Furthermore, when using air conditioning or mechanical ventilation, they must be periodically checked, mantained, cleaned and sanitized for the protectionof workers. Otherwise, ventilation systems may become a source of pollution in the air of workplaces.
Ventilation systems may become a source of pollution:
- when there are lurking pathogens. In this case it is necessary a microbiological investigation to detect the presence of excessive microbial load. If this is traced in the plant or in the air of premises served by the plants, these should be subjected to reclamation.
- when they take the air from polluted areas, for example from exhaust gases. In this case it is necessary an analysis of the particles dispersed in the areas served by the plants and/or toxic gases and/or chemicals responsible for pollution outside.
 In order to assess the overall levels of microbial contamination and therefore to obtain an estimate of the degree of environmental health in the workplace, LABORAD srl carries out the quantitative analysis of:
In order to assess the overall levels of microbial contamination and therefore to obtain an estimate of the degree of environmental health in the workplace, LABORAD srl carries out the quantitative analysis of:
1. Total psychrophilic bacterial load: it is a valid indicator of bacterial contamination of the environment;
2. Total mesophilic bacterial load: it is a valid indicator of contamination from humans and animals;
3. Total fungal load (mold and yeasts): is a very important environmental indicaton, as it is often related to the presence of high humidity and dust, reduced ventilation and poor air quality. Some molds are responsible for infectious diseases in humans, as well as hypersensitivity reactions, allergies or toxicity.
For further informations and for a free evaluation, ask the expert.
Legionella spp
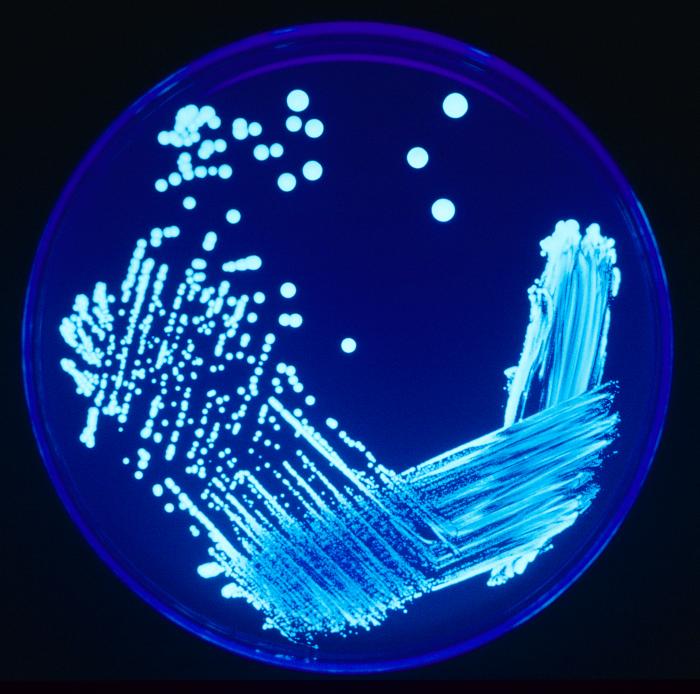 Legionellas are present in natural and artificial aquatic environments: they are found in the springs, including thermal springs, rivers, lakes, steams, land. From these natural environments, they go through pipelines and water systems of buildings, such as tanks, pipes, fountains and pools (they were also detected in mud, clay or terracotta artefacts).
Legionellas are present in natural and artificial aquatic environments: they are found in the springs, including thermal springs, rivers, lakes, steams, land. From these natural environments, they go through pipelines and water systems of buildings, such as tanks, pipes, fountains and pools (they were also detected in mud, clay or terracotta artefacts).
The bacteria remain viable in water at temperatures between 5.7 and 63 °C, while actively develops between 25 and 42 °C (up to 22 °C the bacteria is alive but inactive). Legionella survives both in acidic and alkaline environments, as it can stand pH ranges between 5.5 and 8.1.
The ideal environment for the growth of the bacteria is made up of stagnant water with the presence of deposits and sediments, the presence of biofilms and amoebae. The biofilm is a film of microorganisms (bacteria, algae, protozoa, viruses, etc…) immersed in an organic matrix in which Legionella find sustenance and shelter from concentrations of biocides that would otherwise be able to kill or inhibit the free-living forms. In fact, the ease with which this bacterium reproduces in the natural environment, in contrast to the difficulty to grow on artificial culture media, is largely due to the ability to multiply within ciliated protozoa and amoebae, which constitute a source of nourishment and protection from adverse environmental conditions (temperature and high acidity, the presence of biocides, etc…), thanks to the ability of amoebae to produce forms of resistance such as cysts.
Inside water systems, Legionella can be found both in free form in water or anchored to the biofilm. The zones of proliferation and accumulation of Legionella are found in water and sanitation facilities, inside the pipes (especially if obsolete and full of deposits), or even closed traits (such as storage tanks), kettles, shower heads and shower distribution terminals. Even the emergency water systems, such as decontamination showers, eyewash stations and fire sprinkler systems can be a place of proliferation. In addition, all installations that produce water spray, such as air conditioning, hot water recirculation networks in water and sanitation facilities, are favorable sites for the spread of bacteria. The other facilities where the Legionellarisk is high are the cooling towers in open circuit and closed circuit, where there is nearbythe presence of the shooting or the air intake ducts. The air conditioning systems must be considered too, such as humidifiers/coolers, nebulizers, spray systems. Some cases of Legionellosis have been associated to the presence of decorative fountains in which water is sprayed (especially when these operate intermittently).
REFERENCE LIMITS
Guidelines (Guidelines containing information on legionellosis for operators of tourist facilities and spas – Gazzetta Ufficiale N 28 -Serie Generale- of February 4, 2005 -pag. 54-60 – Italia – Italy) suggest the presence of maximum levels for Legionella in waters over which actions should be taken. These limits refer to:
- cooling towers, for which there is no intervention until 1000 colony-forming units/liter (CFU/L). A value greater than 10000 CFU/L is instead considered a relevant contamination that must lead to an immediate action for cleaning, even in the absence of clinical cases.
- water systems for which the recommended limits are of course much lower: the threshold of non-intervention is set at 100 CFU/L. Exceeded 1000 CFU/L it is necessary to undertake preventive measures and analyze the risk as established in paragraph 3, “Prevention and control of risk from exposure to Legionella” (G.U. N 28 of February 4, 2005). Exceeded the 10000 CFU / L the reclamation becomes, as for cooling towers, immediate and compulsory, even in the absence of clinical cases.
LAWS
Guidelines for prevention and control of legionellosis – Gazzetta Ufficiale N 103 (Serie Generale) of May 5, 2000 (page 12) – Italy



